For more than 50 million Americans, a Medicare Part D plan provides prescription drug coverage. As is often the case with other Medicare options, Part D plans range in both cost and coverage, increasing the complexity when determining which plan best fits the beneficiary’s unique financial and medical needs. While this process may be complicated, it is also incredibly important.
When choosing which plan to enroll in, beneficiaries are urged to consider what coverage the plan provides and where any gaps in coverage may lie. One such common coverage gap was known as the “donut hole,” which will soon be eliminated in 2025.
What Was the Medicare Donut Hole?
The Medicare Part D donut hole, or Medicare coverage gap, referred to the Part D prescription drug coverage stage when Medicare beneficiaries met certain out-of-pocket thresholds and had to pay a larger portion of their prescription drug costs until they reached the catastrophic coverage level. Initially, the cost-share requirements in the donut hole were much higher, with instances of beneficiaries paying 100% of prescription drug costs once they reached this stage.
That share had come down thanks to recent legislative changes. Previously, up to 25% of medication costs had to be covered by those in the donut hole. Planning for potential shifts in out-of-pocket expenses throughout the year became easier when beneficiaries understood the different stages of Part D, including this Medicare coverage gap.
Stages of Part D Prescription Drug Coverage
Medicare Part D plans for prescription drugs previously followed four stages of coverage. This will now be simplified to three. These plans last from January 1st through December 31st and reset the following calendar year:
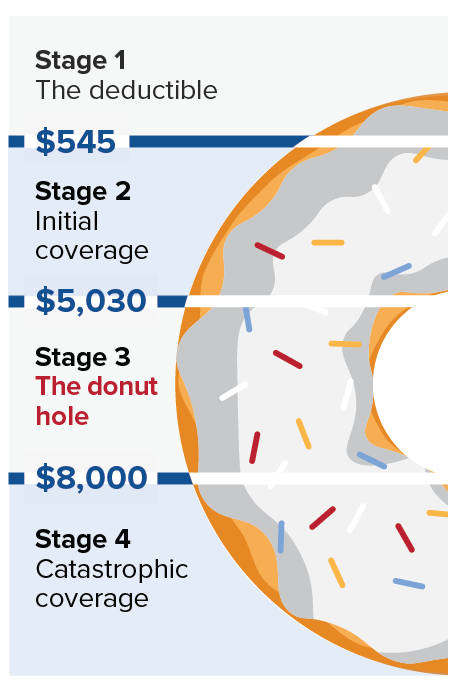 Stage 1 – The deductible requires beneficiaries to pay 100% of prescription costs until they reach a set amount. At that point, the drug plan begins covering its share. Deductibles differ across plans, but a yearly cap is set by the Centers for Medicare & Medicaid Services (CMS) that no plan can exceed.
Stage 1 – The deductible requires beneficiaries to pay 100% of prescription costs until they reach a set amount. At that point, the drug plan begins covering its share. Deductibles differ across plans, but a yearly cap is set by the Centers for Medicare & Medicaid Services (CMS) that no plan can exceed.
Stage 2 – Initial coverage begins once the deductible is met. The drug plan then covers its portion. A fixed amount per prescription is expected for those with copays, while costs may change throughout the year for beneficiaries with coinsurance, depending on drug prices. Coverage shifts into the donut hole once the CMS-mandated maximum is spent by both the beneficiary and the plan.
The out-of-pocket maximum at this stage for 2025 is $2,000 (significantly decreased from $5,030 in 2024).
Stage 3 – After reaching the out-of-pocket cost threshold, beneficiaries enter the catastrophic coverage stage. At this point, they pay nothing for covered Part D drugs and stay in this stage until the next calendar year resets their plan.
The Donut Hole is Gone in 2025!
Stage 3 was formerly known as the “Donut Hole,” which limited how much the drug plan paid for covered prescriptions. The catastrophic coverage stage followed it. Beneficiaries paid up to 25% of drug costs and dispensing fees until reaching the out-of-pocket maximum.
One of the most significant changes for 2025 is the elimination of the “donut hole” or coverage gap. This means that beneficiaries will no longer face a period where they pay a higher percentage of their prescription drug costs before reaching catastrophic coverage. This change, along with the lower out-of-pocket maximum, will significantly reduce prescription drug costs for many Medicare beneficiaries.
Seek Experienced Guidance from Aevo Insurance Services
Contact Advocator Advantage to speak with an experienced licensed insurance agent about your Medicare options, including those for Part D plans. Our Medicare advocacy extends through every step of the enrollment process, starting with assistance in selecting a Medicare plan that meets your medical and financial needs.
This information is up-to-date as of April 2025, based on information made public at that time. For the most recent information, visit the source links.
We do not offer every plan available in your area. Any information we provide is limited to those plans we do offer in your area. Please contact Medicare.gov or 1-800-MEDICARE to get information on all your options.

 Stage 1 – The deductible requires beneficiaries to pay 100% of prescription costs until they reach a set amount. At that point, the drug plan begins covering its share. Deductibles differ across plans, but a yearly cap is set by the Centers for Medicare & Medicaid Services (CMS) that no plan can exceed.
Stage 1 – The deductible requires beneficiaries to pay 100% of prescription costs until they reach a set amount. At that point, the drug plan begins covering its share. Deductibles differ across plans, but a yearly cap is set by the Centers for Medicare & Medicaid Services (CMS) that no plan can exceed.


